Understanding Blood Oxygen Levels
What is Blood Oxygen Level?
Blood oxygen level is the amount of oxygen circulating in the blood. Red blood cells carry most of the oxygen, collecting it from the lungs and delivering it to all parts of the body. A person’s blood oxygen level is an indicator of how well the body distributes oxygen from the lungs to the cells, and it can be important for people’s health.
Ways in measuring your blood oxygen level
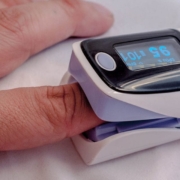
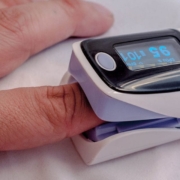
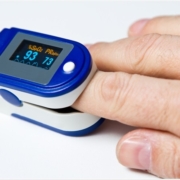
There are two ways in measuring your blood oxygen level, arterial blood gas and a pulse oximeter. An arterial blood gas test is a blood test. It measures your blood’s oxygen level. The test also checks the balance of acids and bases, known as the pH balance, in your blood. An ABG is very accurate, but it’s invasive while the pulse oximeter is a noninvasive device that estimates the amount of oxygen in your blood. It does so by sending infrared light into capillaries in your finger, toe, or earlobe. Then it measures how much light is reflected off the gases. A reading indicates what percentage of your blood is saturated, known as the SpO2 level. This test has a 2 percent error window. That means the reading may be as much as 2 percent higher or lower than your actual blood oxygen level. This test may be slightly less accurate, but it’s very easy for doctors to perform. So doctors rely on it for fast readings.
How blood becomes oxygenated
Understanding how blood is saturated with oxygen begins with the alveoli or air sacs. There are millions of these microscopic air sacs in the lungs. They serve an important function to exchange oxygen and carbon dioxide molecules to and from the bloodstream. When oxygen molecules pass through the alveoli, they bind to hemoglobin which is a substance in the blood. As the hemoglobin circulates, oxygen essentially hitches a ride and gets dropped off to the body’s tissues. With this, hemoglobin picks up carbon dioxide from the tissues and transports it back to the alveoli so the cycle can begin all over again. The level of oxygen in your blood depends on several key factors, how much oxygen you breathe in, how well the alveoli swap carbon dioxide for oxygen, how much hemoglobin is concentrated in red blood cells, and how well hemoglobin attracts oxygen. Most of the time, hemoglobin contains enough oxygen to meet the body’s needs. But some diseases reduce their ability to bind to oxygen.
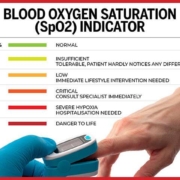
Measuring your blood oxygen levels
Generally speaking, an oxygen saturation level below 95% is considered abnormal and anything below 90% is an emergency. When this happens, oxygen therapy is needed, sometimes urgently. The brain is the most susceptible organ to hypoxia, and brain cells can begin to die within five minutes of oxygen deprivation. Should hypoxia last longer, coma, seizures, and brain death can occur. It is very important to determine the cause of low oxygen saturation in order to correct the problem. With chronic conditions, such as COPD and asthma, the root cause is usually low air exchange in the lungs and alveoli. In addition to oxygen therapy, steroids or bronchodilators may be needed to open the airways.
Treatment
The treatment options for low blood oxygen levels include supplemental oxygen. Doctors can administer oxygen therapy in an office, or they can prescribe or recommend the use of home oxygen therapy. A range of devices is available for delivering and monitoring home oxygen therapy, but some require a prescription. People can make lifestyle adjustments to reduce the symptoms of low oxygen levels, as well as improve their general health and quality of life. Eating a healthy and balanced diet can also help improve blood oxygen saturation. Since iron deficiency is one of the major causes of low oxygen saturation, eating foods that are rich in iron, such as meat, fish, kidney beans, lentils, and cashew nuts, can be helpful.
Disclaimer
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. The purpose of this website is to promote broad consumer understanding and knowledge of various health topics. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition or treatment before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.
References: